Saliva provides a number of important functions, including making eating easier and more enjoyable, facilitating speech and helping maintain oral health. Building on over 100 years of oral healthcare research, we have been investigating saliva.
Recently, the number of people suffering from dry mouth is increasing.
Based on a survey conducted in 2017, we estimate that around 24 million people in Japan ages 20 to 69 regularly experience such symptoms of oral discomfort as dryness and stickiness in the mouth.
Dry mouth (xerostomia) commonly occurs when the amount of saliva secreted in the mouth decreases. This can result from systemic illnesses, such as diabetes and Sjögren's syndrome, an autoimmune disease, pharmaceutical side effects, habitual mouth breathing, smoking and mental stress. Moisture-retentive ingredients, such as hyaluronan, have conventionally been used to relieve dryness in the mouth, but such treatment does not alleviate the decrease in the amount of saliva secreted. Responding to this need, we searched for ingredients that would promote salivation and found that polyglutamic acid (PGA) promotes continuous saliva secretion.
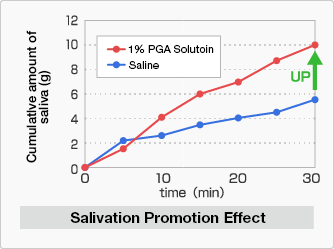
Following 30 seconds of oral rinsing with either normal saline solution or PGA solution, the amount of saliva secreted was measured at five-minute intervals over a 30-minute period to calculate the cumulative amount of secretion. The results showed that, compared with normal saline solution, the amount of secreted saliva increased significantly following rinsing with PGA solution.
Periodontopathic gram-negative bacteria leave behind the toxin lipopolysaccharide (LPS) even after the bacteria themselves are killed. The remaining toxin can then continue to contribute to the progression of periodontal disease symptoms, such as inflammation and tissue destruction. To confirm the exact mechanism behind the relationship between LPS and periodontal disease progression, we conducted an exhaustive genetic analysis (DNA microarray analysis), which found that LPS decreases the expression of genes related to collagen synthesis in human gingival fibroblasts while increasing the expression of genes related to collagen degradation, thus leading to reduced collagen levels in periodontal tissues and tissue destruction.
We then began to look for an ingredient that would inactivate LPS. This led us to lactoferrin, an antibacterial agent present in saliva. By binding to and inactivating LPS, lactoferrin was found to inhibit periodontal tissue destruction, such as collagen degradation caused by LPS.
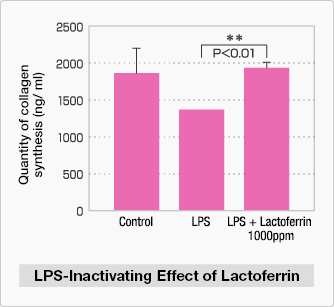
Human gingival fibroblasts were treated with LPS or LPS and lactoferrin and the quantity of type I collagen (the collagen that is a major component of gingival tissue) synthesis was measured. The results showed that type I collagen synthesis decreased in the cells treated with LPS alone, but stayed at a healthy level when lactoferrin was also added.
Reference: Suzuki et al. Potent action of bovine lactoferrin against pathogenesis factors of periodontal disease: alteration of gene expression profiles of human gingival fibroblast by lactoferrin. Lactoferrin 2007. Nihon Igakukan, pp 68-72
During this research into the effectiveness of lactoferrin in preventing periodontal disease, we found a new function of lactoferrin-regulating lipid metabolism-leading to the development of a supplement that helps reduce visceral fat.
Lion has developed and commercialized a saliva testing system, the Salivary Multi Test (SMT), to enable patients to understand their oral conditions through objective data. SMT can measure the levels of six saliva analytes based on chairside measurements that take only five minutes at a dental clinic. Namely; the SMT measures cariogenic bacteria, acidity and buffer capacity as indicators of tooth health; leukocyte and protein levels as indicators of gum health; and ammonia as an indicator of oral cleanliness. The results of these measurements are shown to patients as a radar chart then and there. Patients are able to understand their own oral conditions after an explanation by a dentist or dental hygienist. Lion has demonstrated the correlations between these six saliva analytes and certain oral conditions in clinical trials. For example, a correlation has been demonstrated between probing pocket depth and the leukocyte and protein levels in the saliva.
1. Sample collection

2. Start of Measurement

3. Completion of Measurement
4. Results

The SMT is a simple test comprising three steps: collection, measurement and results, allowing users to immediately see the test results. At dental clinics, the SMT can be used to help understand the oral condition of first-time patients, raise awareness of oral health when patients come in for treatment or check-ups, or increase patients’ motivation to practice self-care. New initiatives using the SMT are also beginning in settings where large numbers of people undergo screenings at once, such as company health check-ups, to aid in the early detection of disease and regular health monitoring. Lion will continue to seek to contribute to preventive dentistry through the SMT.
Back to Science Journal Menu